🔍 Keywords: Audace Pharma, Audace Vietnam, Stages of Cirrhosis, Liver Fibrosis, Liver Symptoms, Causes of Cirrhosis, Metavir Stages, Liver Function Tests, Chronic Liver Treatment, Hepatocellular Carcinoma (HCC), Liver Fibroscan, ALT AST Levels, Specialized Hepatology Care, Cirrhosis Prevention.
-
Definition and Pathophysiological Nature of Cirrhosis
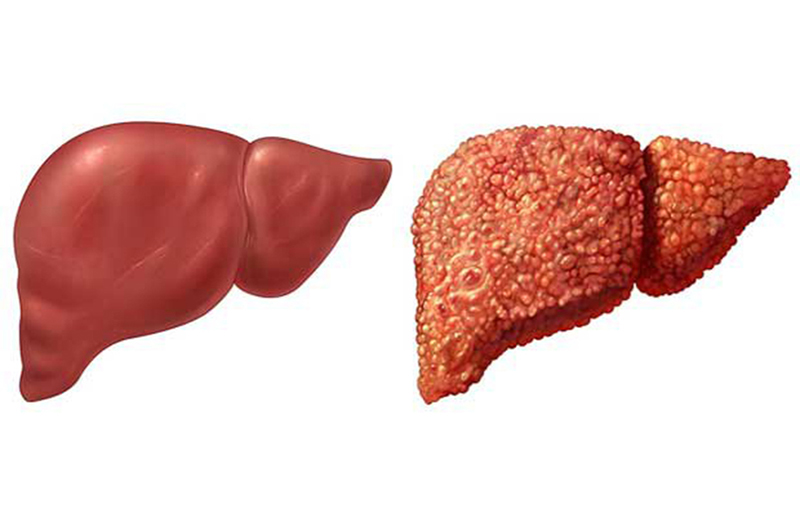
Cirrhosis is the ultimate consequence of long-term, chronic damage to liver cells. From a pathological standpoint, this condition transforms the normal liver architecture into abnormal, nodular structures. The process begins when liver cells are repeatedly injured, triggering the excessive formation of fibrous connective tissue (primarily collagen) to replace dying cells. However, these fibrous tissues lack the metabolic and secretory functions of healthy liver cells. As the fibrous areas expand, they encircle the liver lobules and create regenerative nodules, disrupting the liver’s natural geometry and obstructing blood flow through the organ.
-
Mechanism of Fibrosis and Functional Decline
The process of liver fibrosis is driven by the activation of stellate cells located within the liver sinusoids. In a healthy state, these cells store Vitamin A; however, when stimulated by chronic inflammation, they switch to an “active” state and produce massive amounts of extracellular proteins. This buildup thickens the barrier between the bloodstream and liver cells, blocking the exchange of vital nutrients and oxygen. As a result, the remaining healthy liver cells become nutrient-deficient and gradually weaken, leading to a decline in critical functions such as the synthesis of plasma proteins (albumin) and clotting factors, as well as a reduced ability to neutralize internal and external toxins.
-
Common Causes of the Disease
The leading cause of cirrhosis in many countries, including Vietnam, is infection with Hepatitis B and C viruses. These viruses invade liver cells, multiply, and trigger a long-term immune response, leading to widespread destruction of the liver tissue.
In addition, consuming ethanol (alcohol) in large quantities over a long period causes direct cell poisoning. The process of breaking down ethanol creates highly oxidative byproducts that destroy cell membranes and trigger severe inflammation.
Another rapidly increasing cause is Non-Alcoholic Fatty Liver Disease (NAFLD). This is closely linked to metabolic syndromes, obesity, and insulin resistance. It causes fat (triglycerides) to build up inside liver cells, eventually leading to “steatohepatitis” – a dangerous combination of fatty deposits and liver inflammation.
-
Stages of Cirrhosis (F1 – F4)
4.1. Early Fibrosis and Initial Scarring (F1 – F2)
In the beginning stage, known as F1 (Metavir scale), the damage is still mild. At this point, chronic inflammation triggers the production of tiny collagen fibers around the liver’s entry points (portal tracts). Since the amount of scar tissue is very small compared to the whole liver, the organ continues to perform its detox and metabolic duties normally. Patients at F1 almost never feel symptoms, so it’s usually only caught by chance during routine blood tests or ultrasounds.
As it moves to F2, the scarring is considered moderate. These scar bands start to spread out, but they haven’t yet formed a tight web that cuts off liver function. Even though the internal structure is changing, the healthy liver cells are strong enough to compensate, keeping your enzyme levels stable. This is known as the “Golden Window” for treatment – if the cause (like a virus or alcohol) is removed, the liver can still absorb some of this scar tissue and recover significantly.
4.2. Severe Fibrosis and Bridging (F3)
F3 marks a dangerous turning point called severe fibrosis or “bridging fibrosis.” At this stage, the scar bands are no longer separate; they start connecting to each other, forming “bridges” between different parts of the liver. This breaks down the liver’s natural geometric structure and begins to block blood flow, causing pressure to build up in the liver’s veins.
At stage F3, you might start feeling vague symptoms like constant fatigue, mild indigestion, or a heavy feeling in the upper right side of your belly. This is the sensitive transition period before the liver is officially “cirrhotic.” Medical intervention now requires a strict combination of medication and diet to stop the final stage from setting in.
4.3. Full Cirrhosis and Regenerative Nodules (F4)
When you reach F4, the liver’s structure is completely transformed by regenerative nodules. These are clumps of liver cells trying to regrow, but they are trapped inside a thick mesh of scar tissue, leaving them unable to connect to the blood supply or bile ducts. The liver becomes hard, bumpy, and often shrinks in size. This is “true cirrhosis,” where the liver fails at its most basic jobs: making blood-clotting factors, producing vital proteins (albumin), and cleaning ammonia from the body.
Clinically, F4 starts as “Compensated Cirrhosis” – a fragile balance where the body still functions because of the remaining healthy spots. However, this balance is easily broken by infections or stress. Once the liver can no longer keep up, it enters “Decompensated Cirrhosis,” leading to life-threatening issues like a severely swollen abdomen (ascites), deep yellowing of the skin (jaundice), and internal bleeding. At this point, the scarring is permanent and cannot be reversed by standard medicine.
-
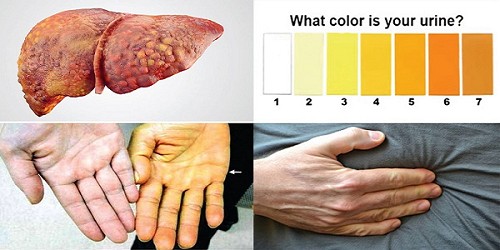
Clinical Symptoms by Progression Stages
In the Compensated Cirrhosis stage, patients often show no obvious symptoms because the healthy part of the liver is still capable of handling necessary functions. Any signs that do appear are usually very vague, such as persistent fatigue, slight weight loss, or mild indigestion.
As the disease progresses to the Decompensated stage, symptoms become much more severe and easier to recognize. Patients may experience jaundice (yellowing of the skin and eyes) due to high bilirubin levels in the blood. Additionally, fluid buildup in the abdomen (ascites) and swelling in the legs (edema) occur. This happens because high pressure in the liver’s veins, combined with a sharp drop in blood protein (albumin), disrupts the body’s fluid balance.
-
Diagnostic Methods and Clinical Evaluation
To accurately determine the level of scarring, modern medicine uses a combination of several methods:
- Blood Tests: These help check liver enzyme levels (AST, ALT), bilirubin, and blood-clotting ability (INR index).
- Imaging Techniques: Tools like abdominal ultrasounds, CT scans, or MRIs allow doctors to see the liver’s shape, detect scar nodules, and look for signs of high vein pressure.
- Fibroscan: This is a non-invasive technique that measures the “stiffness” of the liver tissue. It is widely used because it provides a clear stage of scarring without the need for surgery.
- Liver Biopsy: In specific cases, this remains the “gold standard.” A tiny sample of liver tissue is taken to be examined under a microscope to confirm the exact stage and cause of the disease at a cellular level.
-
Dangerous Complications
If left uncontrolled, cirrhosis leads to complications that directly threaten life. High pressure in the liver’s veins (portal hypertension) forces blood to find alternative routes, causing swollen veins in the esophagus and stomach. These veins are fragile and can easily burst, leading to massive internal bleeding. Another serious issue is Hepatorenal Syndrome, which occurs when liver failure disrupts blood flow to the kidneys, leading to acute kidney failure.
Furthermore, cirrhosis is the leading risk factor for Hepatocellular Carcinoma (HCC), a type of liver cancer. Hepatic Encephalopathy (liver coma) also frequently occurs because the liver can no longer filter ammonia and other toxins, allowing them to enter the bloodstream and attack the central nervous system.
-
Treatment for Cirrhosis
The primary goals of treatment are to slow down the scarring process, prevent complications, and treat the root cause.
- Controlling Viruses: For those with cirrhosis caused by viruses (such as Hepatitis B or C), antiviral medication is the top priority. You can imagine these drugs as a “lock” that prevents the virus from multiplying and attacking liver cells. When the viral load drops to its lowest level, the liver gets a chance to rest and recover, preventing scars from spreading and significantly reducing the risk of liver cancer.
- Stopping Alcohol: If alcohol is the cause, saying “no” to all alcoholic beverages is a mandatory requirement with no exceptions. Alcohol creates toxic substances that destroy the liver directly. Quitting immediately lightens the liver’s detox load and stops inflammation from getting worse. This is the most crucial step to allow other supportive medications to actually work.
- Dietary Management: Patients need a smart menu that provides enough nutrients without overworking the liver. First, reduce salt intake (eat as blandly as possible). Salt is the main culprit behind water retention, which causes abdominal bloating and leg swelling. Second, regarding protein, do not cut it out completely as this leads to malnutrition and muscle loss. However, avoid excess red meat; instead, prioritize protein from fish, eggs, or beans, which the liver can process more easily.
- Liver Transplant: In cases where the liver is too severely damaged to heal and medications are no longer effective, a liver transplant is considered. This method replaces the damaged liver with a healthy one from a donor. Although it is a major and complex surgery, it offers a second chance at life and remains the ultimate solution for patients in the final stages.
PARTNER SOLUTIONS FROM AUDACE PHARMA
Understanding the challenges of cirrhosis and its dangerous complications, Audace Pharma has researched and developed a specialized product ecosystem to support liver cells. With a mission to protect comprehensive liver function and promote natural detoxification, we provide optimal solutions tailored to the specific needs of maintaining and restoring liver health for our customers.
For daily protection and enhancement: Atiso Pluss and Atiso are ideal choices to support daily liver detoxification and maintain overall wellness.
For intensive recovery and symptom support: During stages requiring specialized care or support for hepatitis symptoms, Orthymin Pluss, Nifamin Gold, and Livernifa serve as reliable companions to strengthen and revitalize liver health.
The journey to control liver disease requires perseverance, and Audace Pharma is proud to empower you with standard medical-grade solutions. Let us help you build a solid protective barrier for your liver starting today.
Don’t hesitate to contact Audace Pharma to co-create sustainable solutions for liver protection and healthcare.
—————————-
𝐀𝐔𝐃𝐀𝐂𝐄 𝐏𝐇𝐀𝐑𝐌𝐀 – 𝐓𝐡𝐞 𝟏𝐬𝐭 𝐏𝐫𝐨𝐟𝐞𝐬𝐬𝐢𝐨𝐧𝐚𝐥 𝐏𝐡𝐚𝐫𝐦𝐚𝐜𝐞𝐮𝐭𝐢𝐜𝐚𝐥 𝐃𝐞𝐯𝐞𝐥𝐨𝐩𝐞𝐫 𝐀𝐠𝐞𝐧𝐜𝐲 𝐈𝐧 𝐕𝐢𝐞𝐭𝐧𝐚𝐦
📞 Hotline: (+84) 961 626 691
📍 Website: audacepharma.com
📩 Email: [email protected]